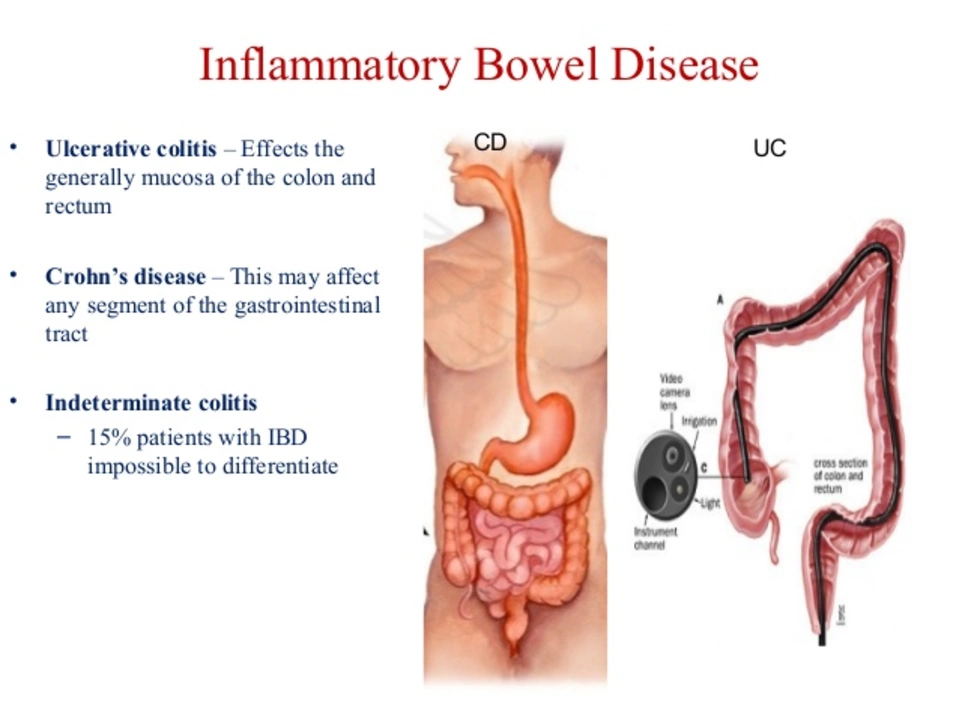
If you’ve heard the term IBD and wonder if it applies to you, you’re in the right place. Inflammatory bowel disease is a catch‑all name for two main conditions – Crohn’s disease and ulcerative colitis – that cause chronic inflammation in the digestive tract. Both can flare up suddenly, make everyday life uncomfortable, and need ongoing care.
First off, know that IBD isn’t an infection you catch from someone else; it’s a mix of genetic, immune and environmental factors that trigger your gut to overreact. That means you won’t get rid of it with antibiotics alone. Instead, managing IBD involves a combination of medicine, diet tweaks, and regular check‑ups.
The warning signs differ a bit between Crohn’s and ulcerative colitis, but many overlap. Common complaints include abdominal pain, cramping, frequent diarrhea (sometimes with blood), urgent bathroom trips, and unintentional weight loss. Fatigue is another big one because your body spends energy fighting inflammation.
Extra‑intestinal symptoms can pop up too – joint aches, skin rashes, or eye irritation. If any of these sound familiar and last more than a couple of weeks, it’s worth talking to a doctor who can run blood tests, stool checks, and imaging studies like colonoscopy to confirm IBD.
Medication is the backbone of IBD control. Doctors often start with anti‑inflammatory drugs such as mesalamine or corticosteroids for short bursts. If those aren’t enough, immunosuppressants like azathioprine or biologics (e.g., infliximab) target specific parts of the immune system to keep flares at bay.
Alongside meds, diet plays a practical role. While there’s no one‑size‑fits‑all IBD diet, many people feel better by avoiding high‑fiber foods during flare‑ups, limiting dairy if lactose is a problem, and staying hydrated. Keeping a food diary can help you spot trigger items.
Stress isn’t the cause of IBD, but it can worsen symptoms. Simple stress‑relief habits – walking, meditation, or short breathing exercises – often make a noticeable difference during tough days.
Regular monitoring is key. Schedule routine blood work and colonoscopies as your doctor advises to catch any complications early, such as strictures, fistulas, or an increased risk of colon cancer.
If you’re newly diagnosed, remember that IBD treatment isn’t static. Your doctor may adjust doses, swap medications, or add new therapies based on how you respond. Don’t hesitate to ask why a change is suggested – understanding the plan helps you stick with it.
Finally, lean on community resources. Support groups, online forums, and patient education sites (like PharmaPassport.com) offer real‑world tips from people walking the same path. Sharing experiences can give you practical ideas for meal planning, symptom tracking, and coping strategies.
Living with inflammatory bowel disease takes effort, but with the right meds, diet tweaks, and a proactive mindset, many people lead full, active lives. Keep an eye on your body, stay in touch with your healthcare team, and remember that each small step adds up to better control over time.